Surprise Location
How Often Should You Have Your A1C Checked?
Your A1C is one of the most informative numbers in diabetes care, but it’s often misunderstood, infrequently tracked, or simply overlooked until something goes wrong. It doesn’t measure how your blood sugar looked this morning. It reflects your average blood glucose control over the past two to three months, making it a reliable window into how well your management plan is actually working day to day. For anyone living with diabetes or prediabetes, knowing how often this test should happen isn’t just a logistical question — it’s a health priority.
The answer depends on where you are in your treatment, how stable your numbers are, and what your care team observes at your visits.
What the A1C Test Measures
The A1C test can be used to diagnose diabetes or to help you understand how your treatment plan is working by providing a picture of your average blood glucose over the past two to three months. That three-month window exists because the test measures how much glucose is attached to hemoglobin — the protein inside red blood cells, which live for roughly that long before being replaced.
For patients working with Dr. Majhail on diabetes management in Surprise, this test forms the backbone of every treatment conversation. It confirms whether your current approach is protecting you from long-term complications or whether adjustments are needed. A single blood glucose reading tells you about one moment in time; your A1C tells you about a whole season of your health.
The higher the A1C percentage, the higher your blood glucose levels have been over the past two to three months, and the greater your risk of developing diabetes complications. Those complications include nerve damage, kidney disease, vision loss, and cardiovascular disease — all of which develop gradually and silently before they become obvious.
So, How Often Should You Get Tested?
The honest answer is that there is no single right answer for everyone. Testing frequency is individualized based on your current control, your treatment plan, and whether anything in your health picture has changed recently. That said, the American Diabetes Association’s 2024 Standards of Care offer a clear framework to start from.
If You’re Meeting Your Treatment Goals
For patients meeting their treatment goals, the ADA recommends having an A1C test at least twice per year. That translates to roughly every six months — a cadence that keeps you and your care team informed without testing more frequently than necessary. If your numbers have been consistently in range and your lifestyle and medications haven’t changed, twice a year gives you enough data to stay on track.
If Your Control Is Unstable or You’ve Changed Treatment
The 2024 ADA guidelines updated their recommendations to include more frequent glycemic assessment for populations that need closer monitoring. Practically speaking, this means quarterly testing (every three months) is appropriate when your A1C is above the normal range, you’ve recently started a new medication, changed your dosage, significantly shifted your diet, or experienced a major health event. Testing every three months gives your care team a real-time look at whether those changes are actually working.
If You Have Prediabetes
People with prediabetes should be tested at least annually — though some people with multiple risk factors may benefit from more frequent monitoring. Prediabetes is a critical window. It’s the stage where thoughtful lifestyle changes can genuinely prevent or delay the onset of type 2 diabetes, and tracking your A1C helps confirm whether those efforts are moving things in the right direction.
What A1C Goals Look Like in Practice
A target A1C below 7% is the standard goal for most non-pregnant adults with diabetes, according to the ADA. But that target isn’t universal.
Older adults who are healthy, with few and stable chronic conditions, and have intact cognitive function should have an A1C goal below 7.0–7.5%. Older adults with more complex health situations or multiple chronic diseases should have individualized, less stringent goals below 8.0%. This nuance matters because pushing A1C too low in someone prone to hypoglycemia can actually create additional risks — and Dr. Majhail’s approach to setting your personal target accounts for your full health picture, not just the number on its own.
A more stringent A1C goal of below 6.5% could be reasonable for some individuals if it can be achieved without significant hypoglycemia or adverse effects on overall well-being.
What Affects Your A1C Between Tests
Your A1C reflects three months of real life, which means it’s sensitive to the daily patterns that don’t always make it into a doctor’s visit. Several factors influence the number:
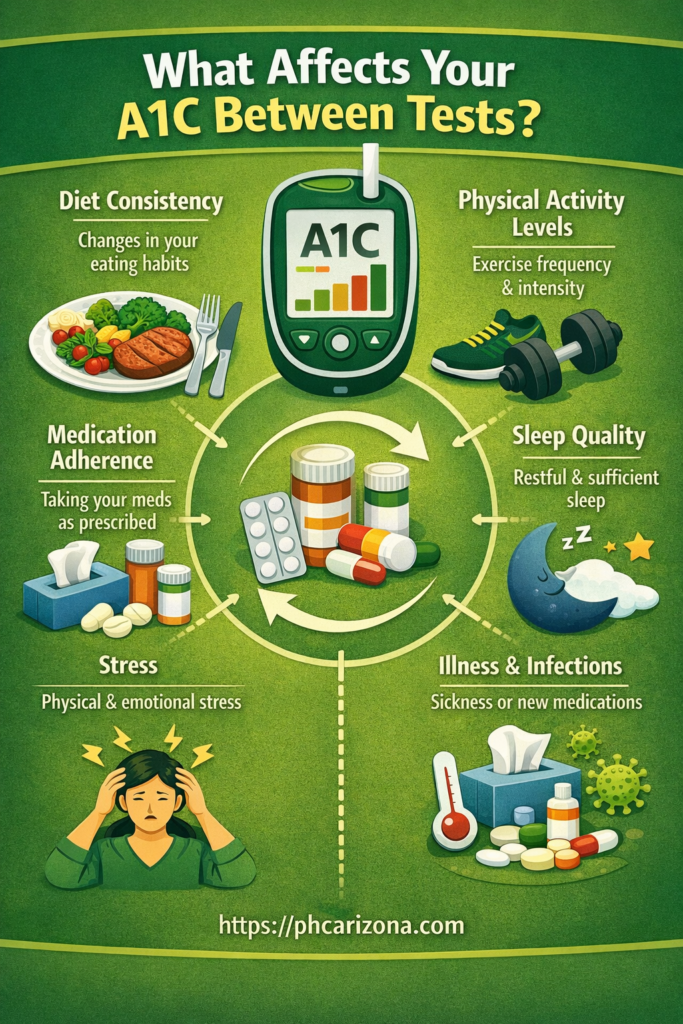
- Diet consistency, particularly carbohydrate intake and meal timing across the full three-month period
- Physical activity levels, which directly affect insulin sensitivity
- Medication adherence — missed doses or inconsistent timing show up in A1C results
- Sleep quality, which affects cortisol levels and blood glucose regulation
- Stress, both physical and emotional, which elevates blood sugar through hormonal pathways
- Other health events, including illness, infections, or new medications that interact with glucose metabolism
This is why A1C visits are most useful when they’re paired with a real conversation about what the past three months actually looked like — not just a number review.
Beyond A1C: What Else Gets Monitored
A1C is central to diabetes management, but it doesn’t capture everything. The 2024 ADA Standards of Care revised the glycemic assessment section to include discussion of continuous glucose monitoring metrics and the benefits and limitations of alternative glycemic markers alongside A1C. For some patients, continuous glucose monitoring (CGM) provides additional daily insight that A1C alone cannot — particularly for catching high and low spikes that average out in the A1C result.
Dr. Majhail may also review kidney function, blood pressure, cholesterol, and eye health at appropriate intervals, because diabetes management is never just about one number. It’s about keeping every system that diabetes can affect in the best possible condition over the long term.
Your A1C is only as useful as the follow-through behind it. If you’re managing diabetes or prediabetes and want a clear, current look at where you stand, schedule an appointment with Dr. Majhail at Physicians Health Center today.
People Also Ask
Yes, and this is one of the known limitations of the A1C test. Because it reflects an average, frequent blood sugar spikes and lows can cancel each other out, producing a result that looks acceptable on paper. This is one reason why continuous glucose monitoring is increasingly used alongside A1C for patients whose daily patterns suggest more variability than their A1C implies.
No. Unlike fasting blood glucose tests, the A1C test does not require you to fast before your blood draw. You can eat and drink normally before the test, making it more convenient to schedule at any point during a regular visit.
Yes. In the presence of hemoglobin variants, pregnancy, glucose-6-phosphate dehydrogenase deficiency, and other conditions that may alter red blood cell turnover, plasma glucose levels are preferred over A1C for monitoring glycemic status, as these conditions can cause A1C results to be misleadingly high or low. If you have any of these conditions, your care team will use alternative measures to track your glucose control.
A daily blood glucose reading captures your sugar level at a single point in time — that morning, after a meal, before bed. A1C reflects your average blood glucose level across two to three months. Both are useful, but they answer different questions. Daily readings help you manage moment-to-moment, while A1C tells you whether your overall strategy is working.
Absolutely. Because A1C reflects a rolling three-month average, consistent changes in diet, activity, medication adherence, and stress management show up in your next result. Many patients see meaningful A1C improvements within a single testing cycle when they make targeted adjustments with their care team’s guidance. The key is consistency across the full period — not just in the days leading up to your appointment.